One Outpatient Procedure. Lasting Lung Health.
The dNerva® Lung Denervation System is a novel, catheter-based system used to treat overactive airway nerves in a procedure called Targeted Lung Denervation. This first-of-its kind technology addresses underlying COPD pathophysiology to help preserve lung health.1,2
Targeted Lung Denervation
Disrupting Pulmonary Nerve Input
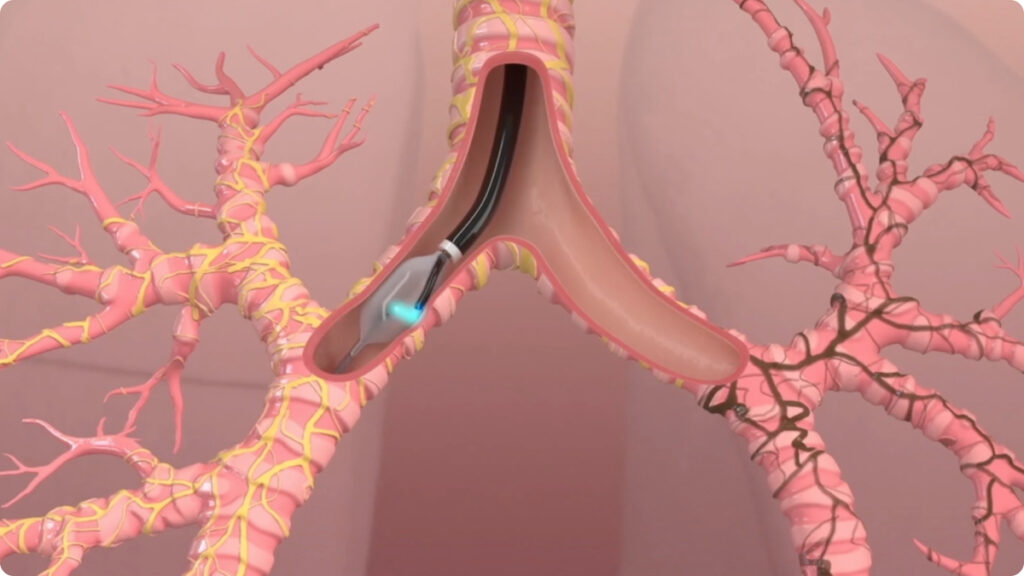
Targeted Lung Denervation (TLD) is an outpatient procedure that involves passing the specialized, dNerva Catheter through a flexible bronchoscope to complete a full circumferential ablation in the main bronchi of each lung.
The ablation permanently disrupts pulmonary nerve input to the lung to reduce the clinical consequences of neural hyperactivity.
Non-Surgical, Outpatient Treatment
The Procedure
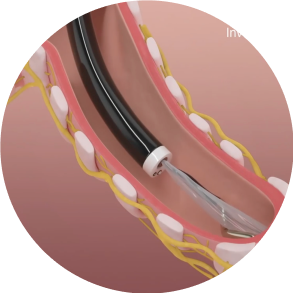
Step 1: Position
The dNerva Catheter threads through the working channel of the bronchoscope and is positioned in the main bronchi.
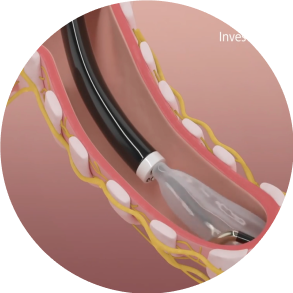
Step 2: Inflation
The conduit and balloon are inflated by circulating the coolant through the catheter which brings the electrode in contact with the airway wall.
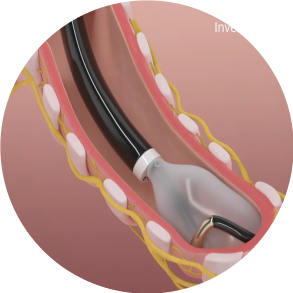
Step 3: Confirmation
Confirm good contact of the electrode with the airway wall and that adequate distance from the esophagus is achieved.
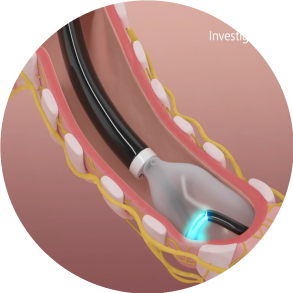
Step 4: Activation
Activation of the radio-frequency energy lasts approximately 2 minutes per position. Each bronchus is treated four times to complete circumferential ablation.
Post-Procedure
The procedure will last about 70-100 minutes and patients can expect to go home the same day. Post-procedure follow-up care is consistent with advanced bronchoscopic procedures.
Reducing Neural Hyperactivity
How it Works
COPD
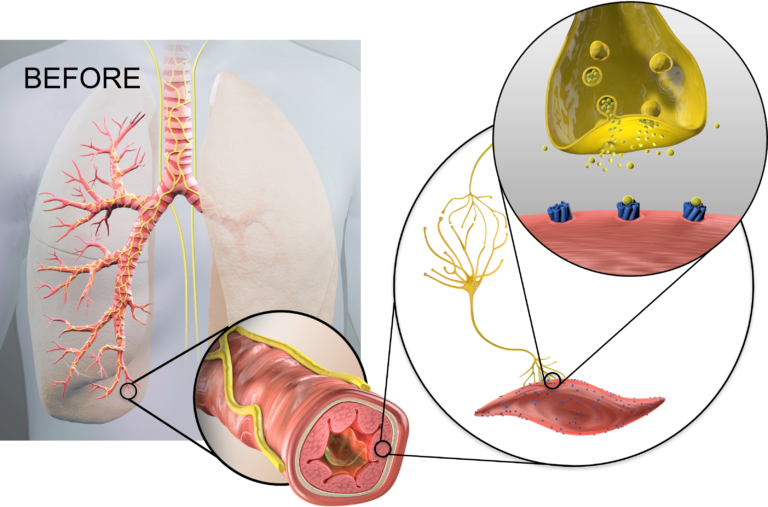
The natural release of acetylcholine in COPD patients occurs when the brain signals the lung, via the vagus nerve, and moves the pulmonary system to a state of heightened neural activity which is associated with chronic airway inflammation, increased exacerbations and symptom burden. 3,24
Anticholinergic Drugs
Current anticholinergic drug therapies attempt to block the binding of acetylcholine in the lungs, helping to reduce COPD symptoms. However, these therapies are not always effective at preventing severe symptoms or exacerbations.
Targeted Lung Denervation
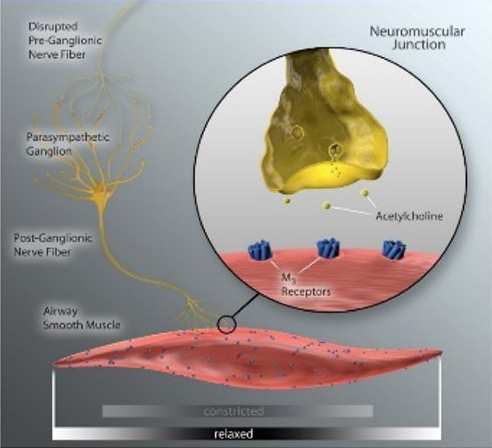
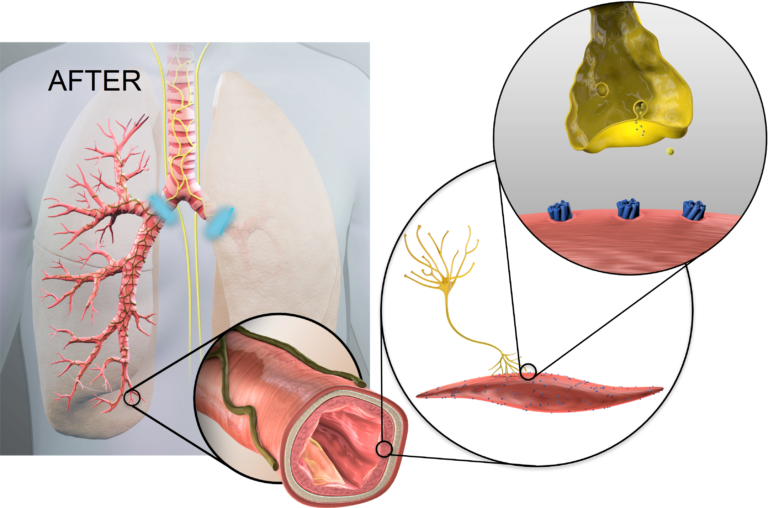
Disruption of vagus nerve signaling as a result of TLD, can durably reduce acetylcholine release, and therefore, keeps the pulmonary system in a state of reduced neural activity.
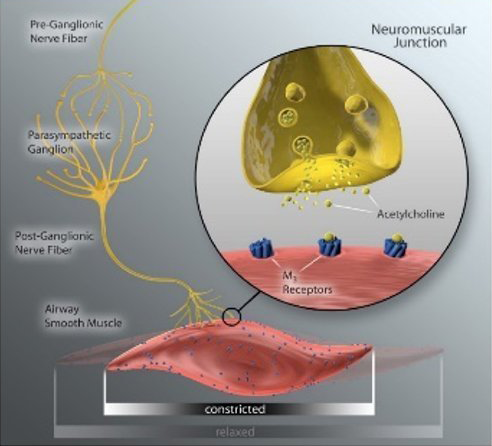
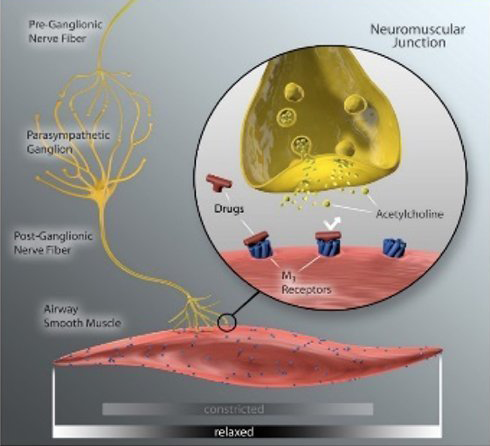
Before & After Slider
The dNerva Difference
With less acetylcholine release, the airway smooth muscle relaxes and mucous secretion decreases moving the pulmonary system to a state of “low alert”. This has the potential to reduce exacerbation risk, improve COPD symptoms and stabilize lung function over time.
Discover our Products
dNerva Lung Denervation System
The dNerva Lung Denervation System is comprised of two parts: The Nuvaira Console and the dNerva Catheter.

Nuvaira Console
The Nuvaira Console includes a thermoelectric plate and pump that cools the fluid circulating through the dNerva catheter to protect the airway wall during Radio-frequency energy delivery. The Nuvaira Console also includes graphical user interface with a prompt screen to control the console and guide the user.
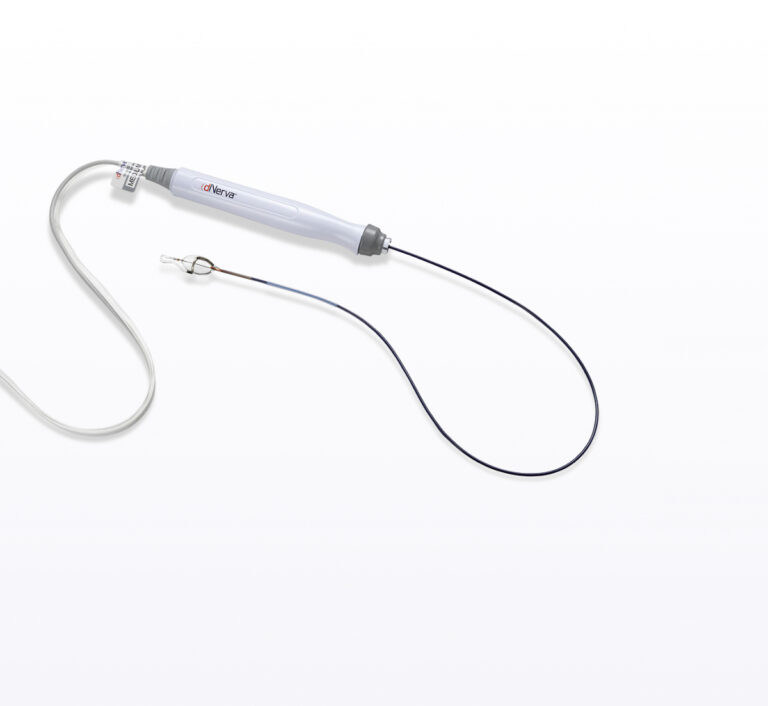
dNerva Catheter
The dNerva Catheter is a specialized, patented disposable component that is compatible with most flexible bronchoscopes utilizing working channels down to 2.8mm in diameter. The distal balloon and electrode assembly have been designed to collapse to fit through the bronchoscope’s working channel. The catheter is available in multiple sizes.
Esophageal Cooling Catheter
The esophageal cooling catheter is designed to regulate the temperature of the esophagus during ablation procedures.
dNerva Lung Denervation System
Design Features
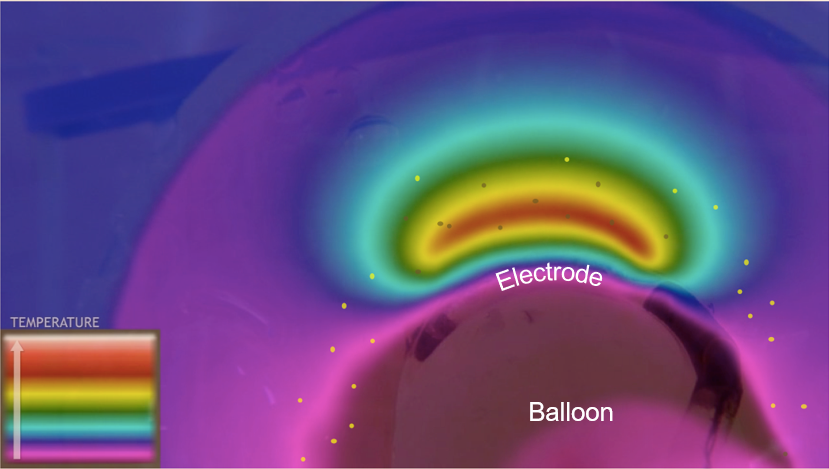
Cooling to Protect Airway Walls
During inflation of the dNerva Catheter, coolant flows underneath the electrode and through the catheter balloon which cools and protects the inner surface of the airway wall while focusing heating at depth.
COPD Exacerbations are the Problem.
Be a Part of the Solution.

The AIRFLOW-3 Clinical Trial is the first interventional COPD device trial targeting exacerbation risk reduction in patients on optimal drug therapy.